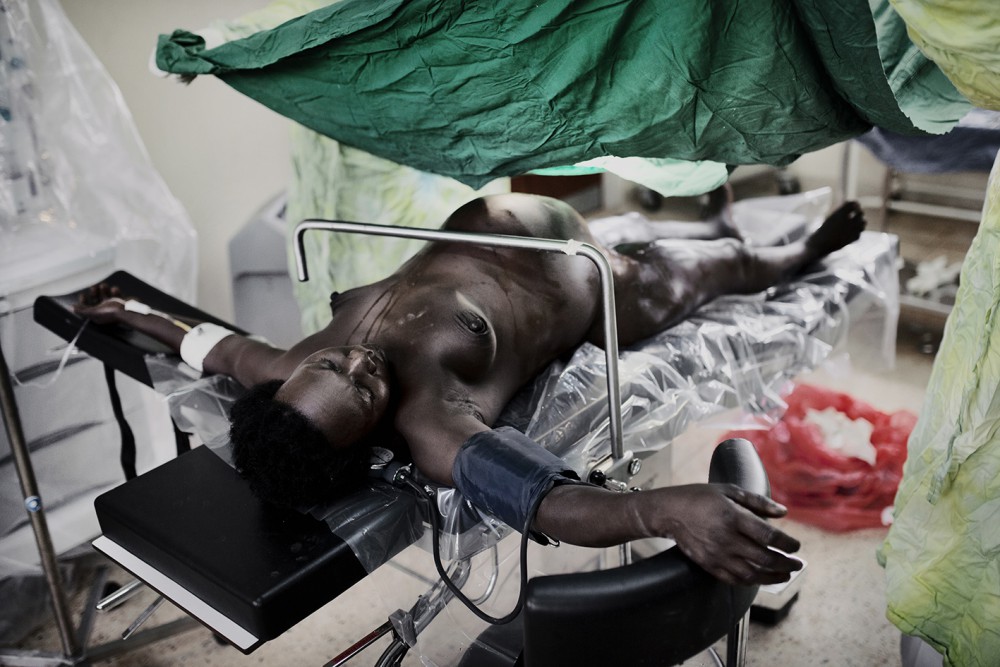
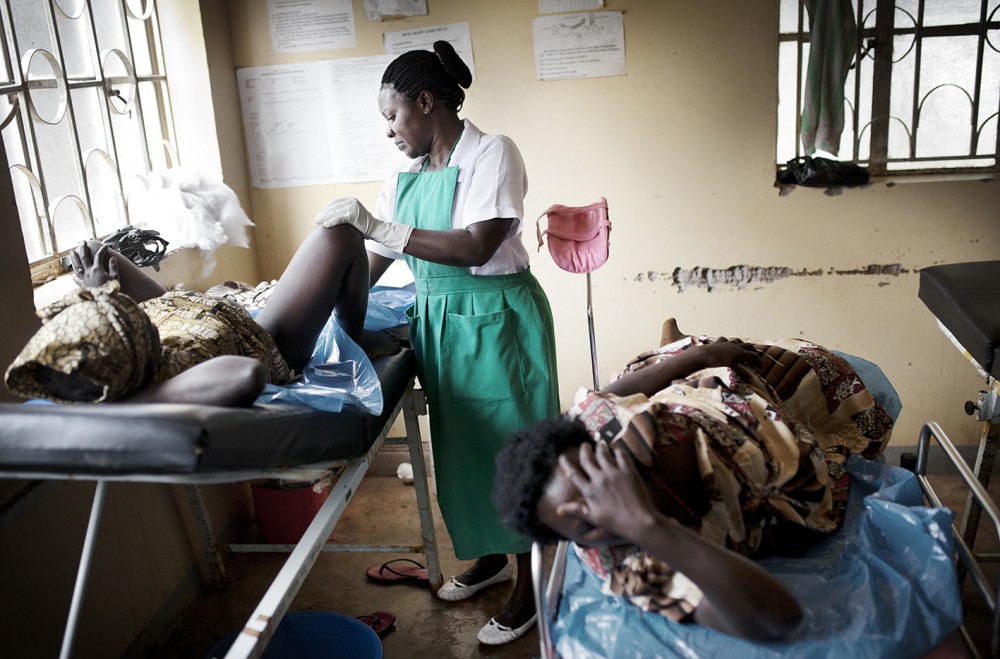
Every day, 800 women die because they are pregnant. More than half of the deaths occur in rural Sub-Saharan Africa, where the chance of surviving childbirth is the lowest in the world. A lack of transport and poor access to adequate healthcare means many women bleed to death.
In Uganda, official statistics claim 310 women per 100,000 live births die from complications at childbirth. But according to Dr John Bosco Serebe, District Health Officer in the Kyankwanzi district in western Uganda, many deaths in the community remain “unnoticed and unregistered.”
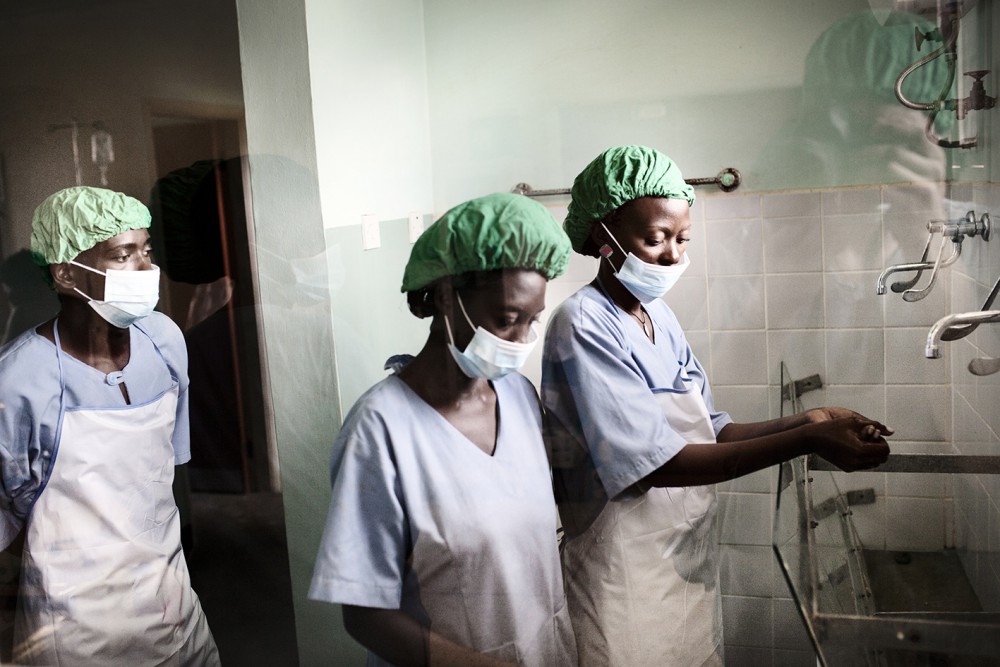
A few years ago, Ugandan authorities banned traditional birth attendants − who have played in central part in the country’s maternal care since the early 1980s − as a response to the high mortality rates. But the country lacks 1 500 midwives and many rural clinics are understaffed.
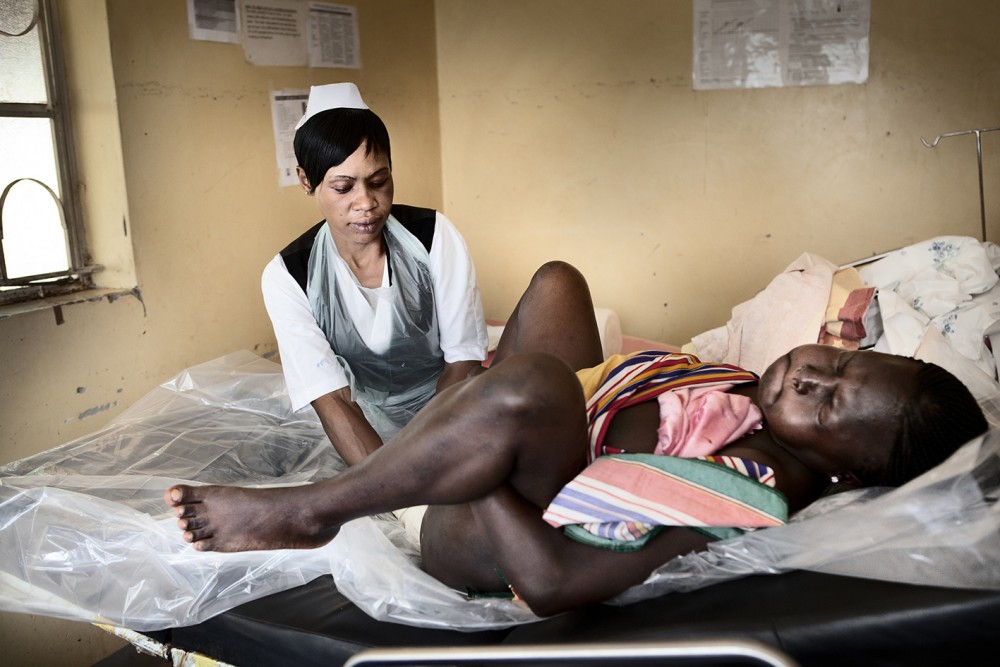
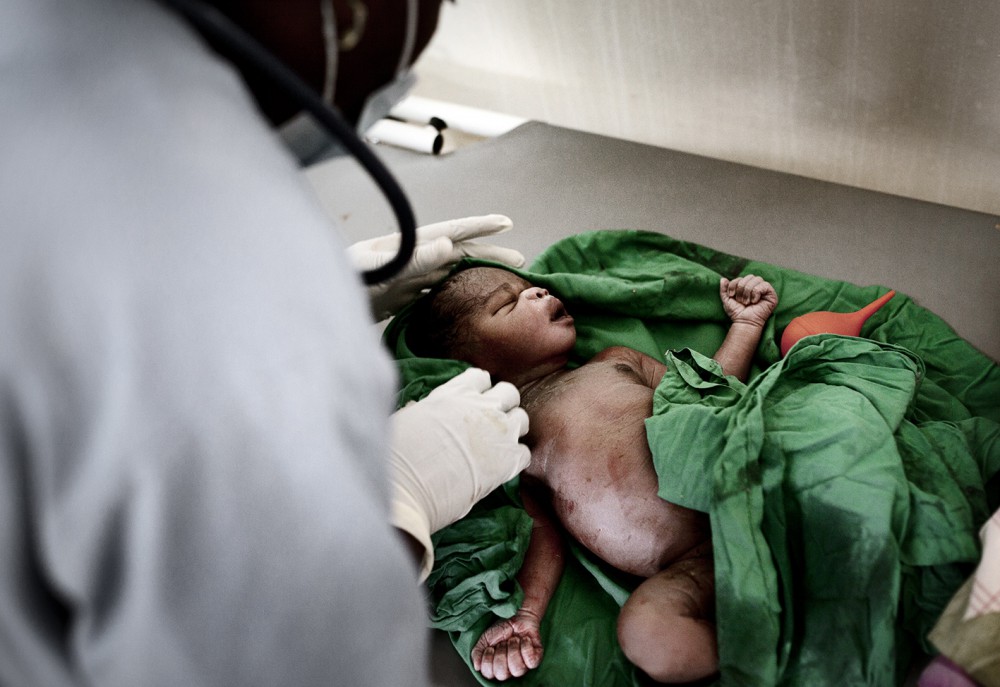
At Ntwetwe Health Centre, three hours’ drive from Kampala, 36-year-old Annet Namata has come to deliver her sixth child. A year ago, she would have been just another statistic. Her baby is breached and the umbilical cord is been wrapped around its neck. Last year, the young doctor would not have had a choice but to send the heavily pregnant mother to Kiboga hospital, a two hour drive along a dirt track. “By that time she would have a ruptured uterus,” says Dr Gordon Mayengo, the only doctor in Ntwetwe.
But Annet is lucky. The small clinic has been equipped with an operating theatre and the medical team are able to perform a Caesarean to get the baby out. The theatre still lacks running water and electricity, but at least there is equipment to perform life-saving surgery. A few hours after surgery, Annet recovers from her ordeal. She is exhausted, but happy to be alive. “I want to continue to have babies for as long as I able to, but after this I’m a bit scared,” she says.
Published: